Autoimmune Skin - Overview of These Skin Conditions
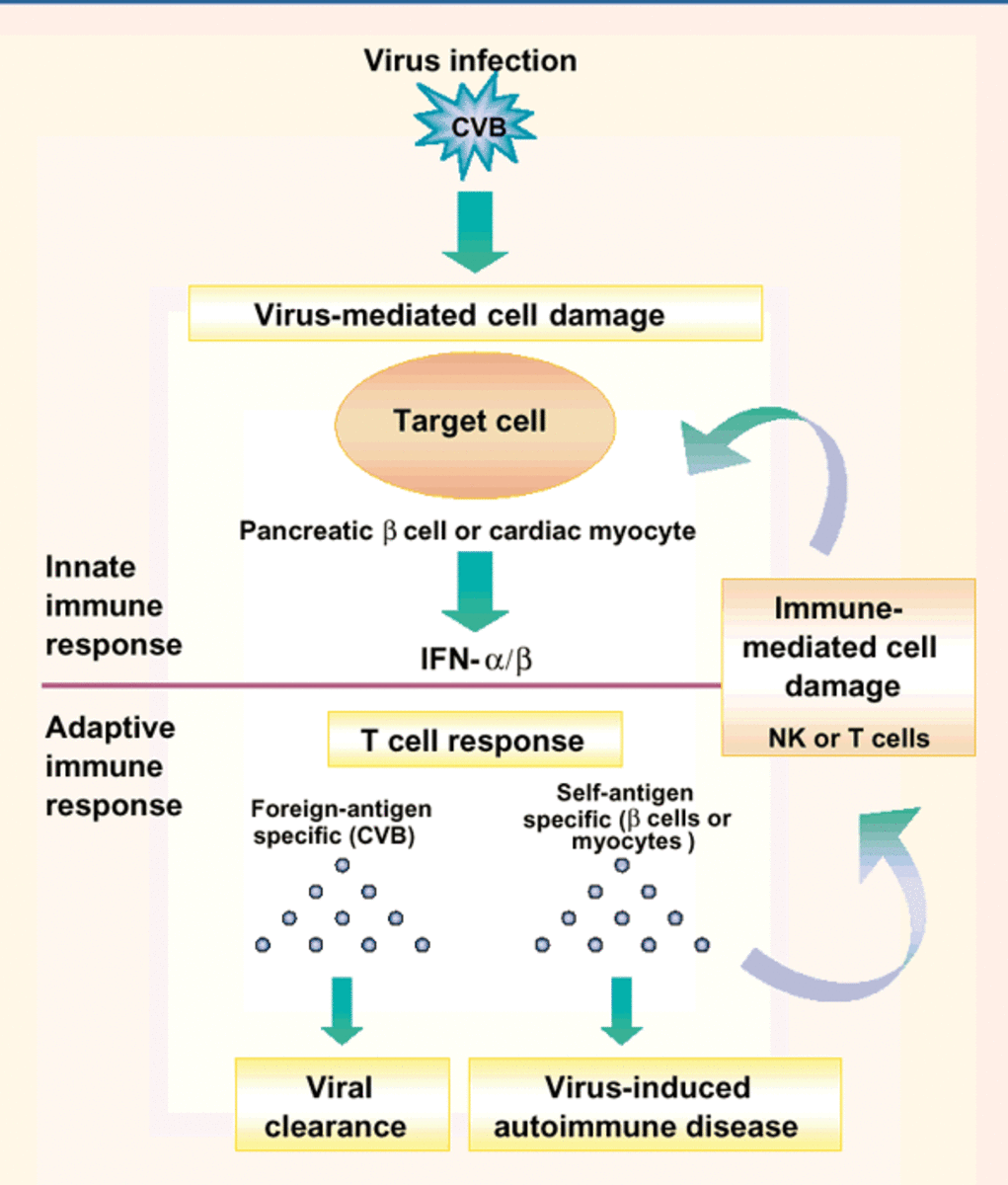
Autoimmune skin conditions can be isolated problems just on the skin or it can be a symptom of a more all-encompassing autoimmune disease. When the immune system targets otherwise healthy tissue, when it is supposed to target diseases and unknown invaders, it is considered an autoimmune condition. They appear in several different varieties and are frequently misdiagnosed or left untreated because the initial impacts mimic more common skin diseases. As with any skin disease, it is critical to properly treat it because damaged skin can worsen the condition and lead to infections.
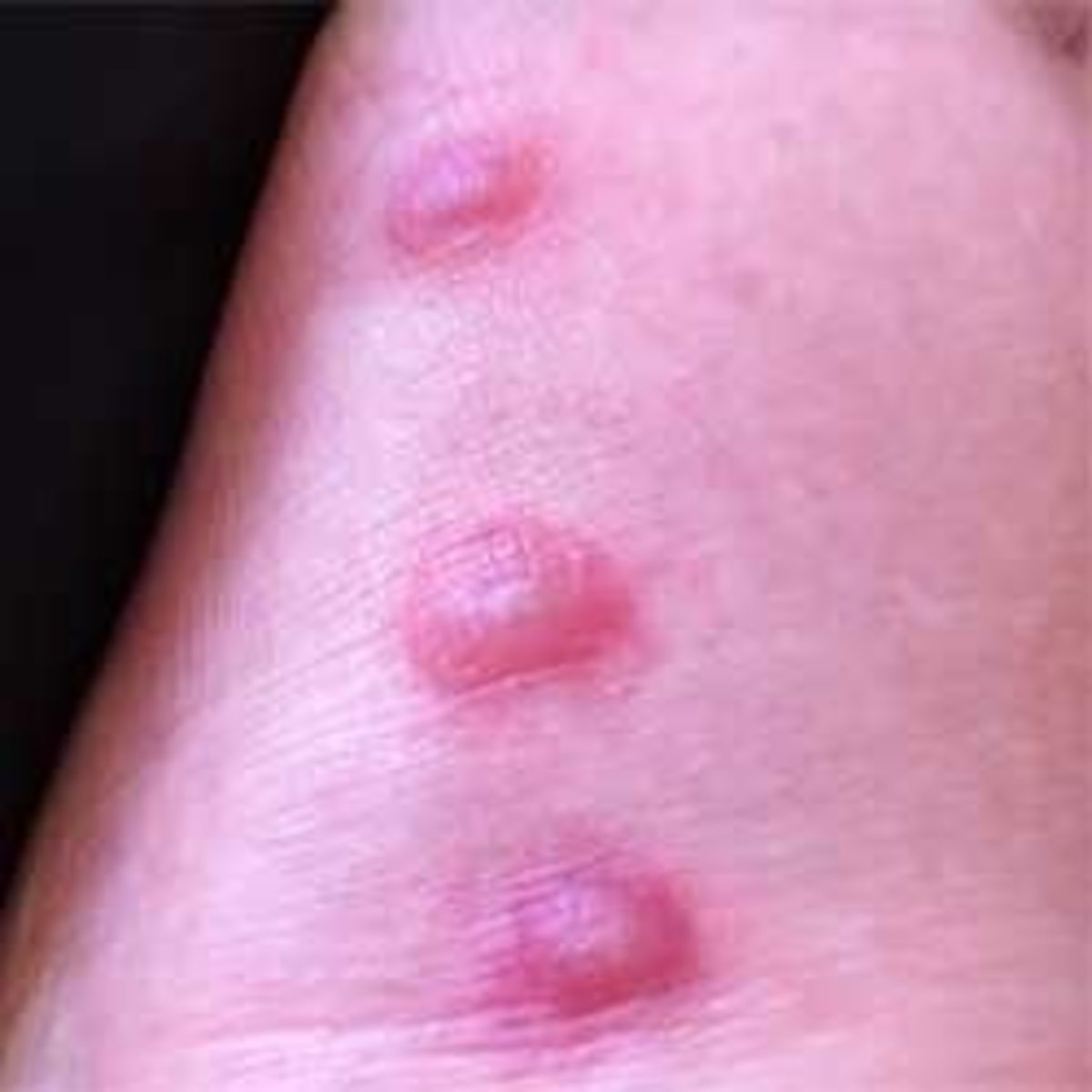
Autoimmune blistering conditions, or bullous skin diseases, are the most typical kind of autoimmune diseases that affect the skin. In these particular situations the proteins that hold an individual's skin cells together are attacked by the immune system. Lesions and blisters are the consequence. Although skin issues are commonly associated with lupus, only 5 percent of lupus patients suffer through bullous skin symptoms. Ladies between the ages of 20 and 40 are most in jeopardy for bullous disorders.
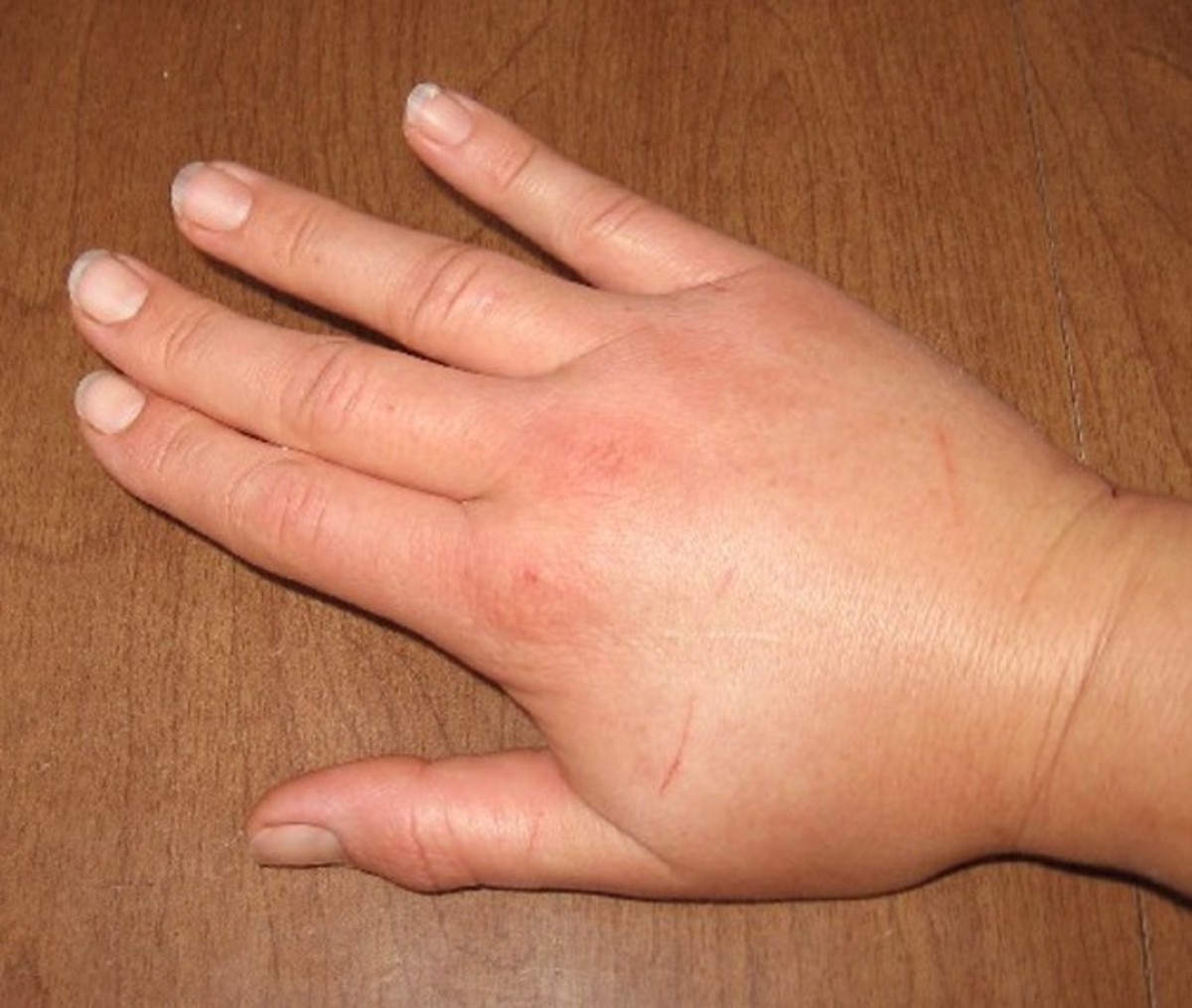
Fluid filled blisters on the body is a disorder known as bullous pemphigoid. Blisters usually occur on the arms, legs or torso and older adults are at the highest risk for the condition. This is a chronic condition meaning it persists for years, often with periods with no blisters followed by flair-ups when blisters appear. Medications to inhibit the immune system and therefore keeping it from leading to this skin disease are what most doctors will prescribe if the condition is serious enough. The side effects can be that your immune system becomes too weakened manage everyday threats like germs and bacteria. Corticosteroids are treatments that are also used which relieves inflammation.
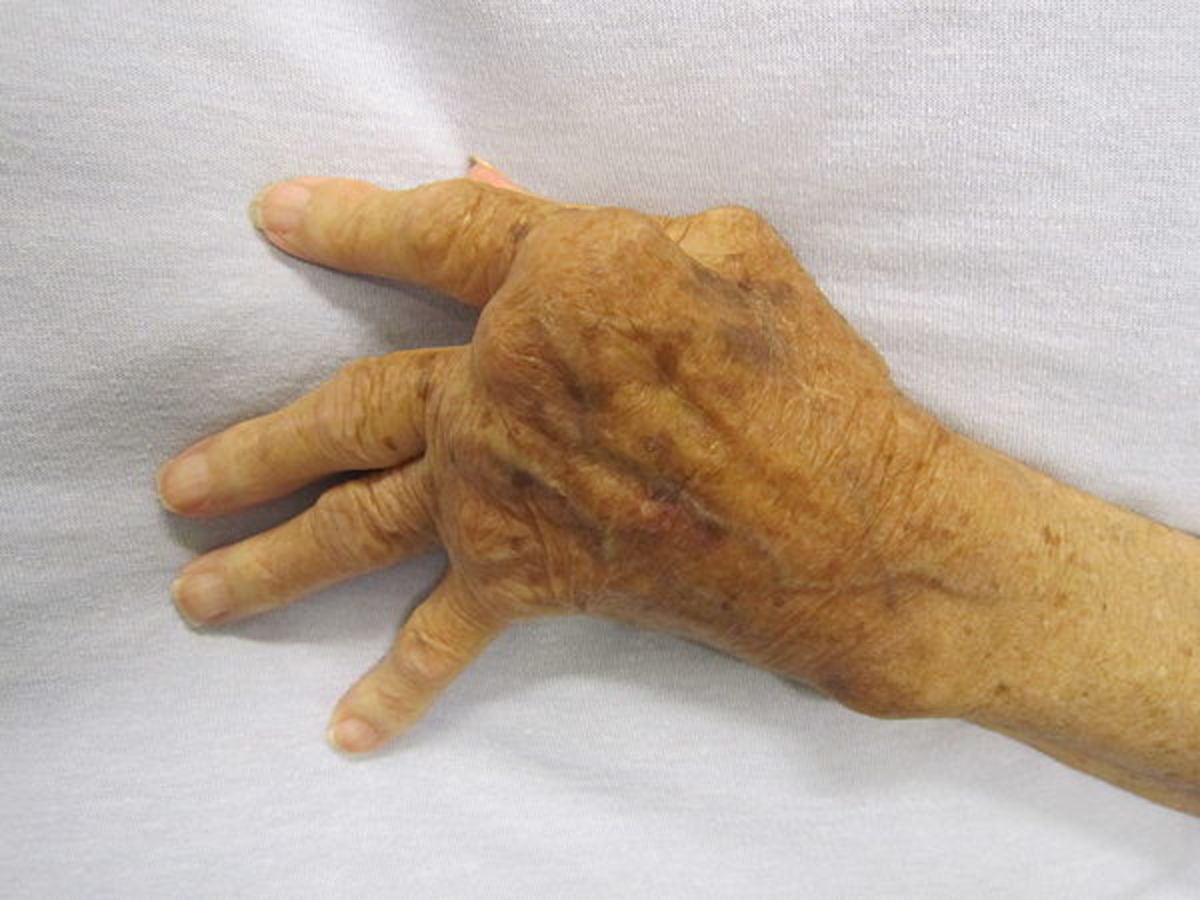
Dermatitis herpetiformis is an autoimmune skin disease that targets those with gluten intolerance or celiac disease. People with celiac disease are unable to digest the gluten protein that is present in grains such as wheat, rye and barley. Itchy blisters and hives will form commonly on a person’s back or buttocks; this disorder is handled by removing all gluten containing products from a person's lifestyle. People with hypothyroidism, Sjogren’s disease or rheumatoid arthritis are also known to get this skin condition.
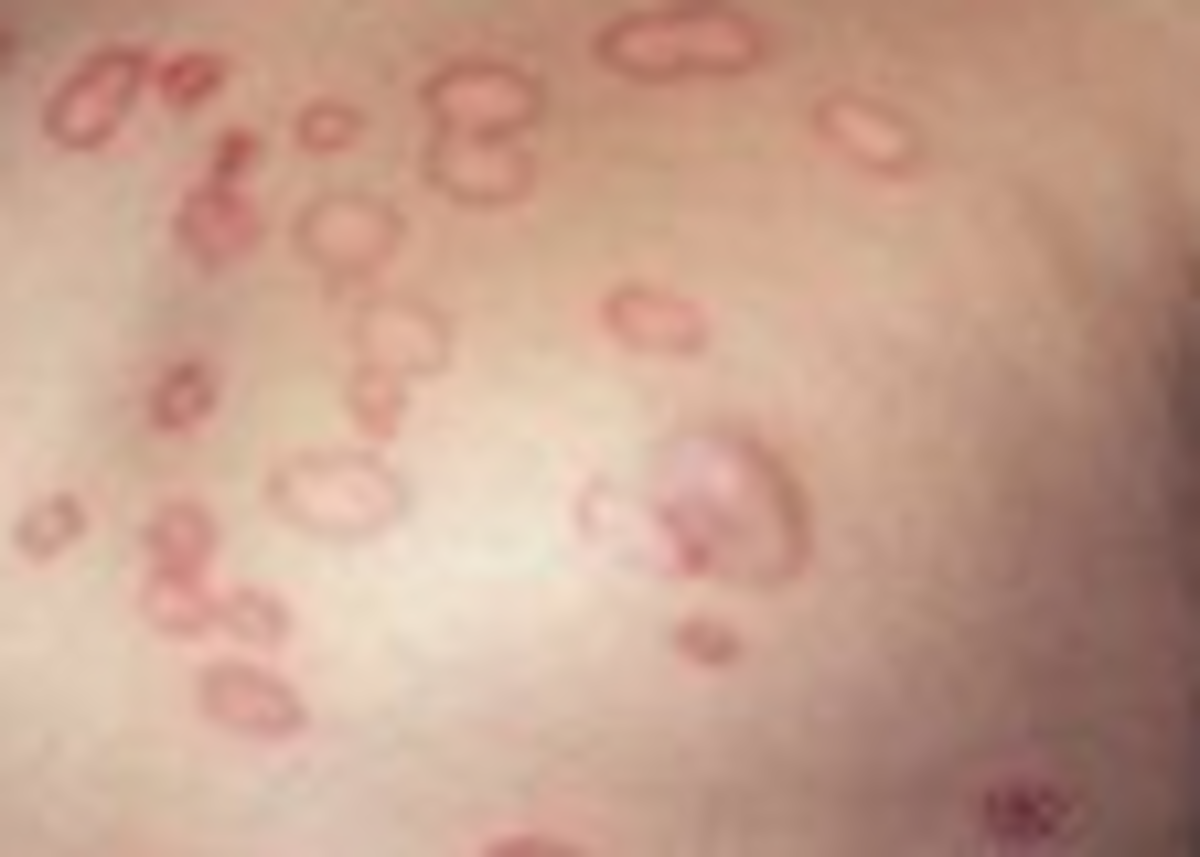
Lichen planus appears together with other autoimmune conditions. This skin condition can strike those with alopecia (hair loss), autoimmune hepatitis, lupus, scleroderma and any number of other conditions. This condition causes small erosive purple lesions. These lesions usually cluster together and often shows up on on the shins, heels or ankles or on the insides of the forearms and wrists. Oral lesions are diagnosed in about 75% of those with the disease.
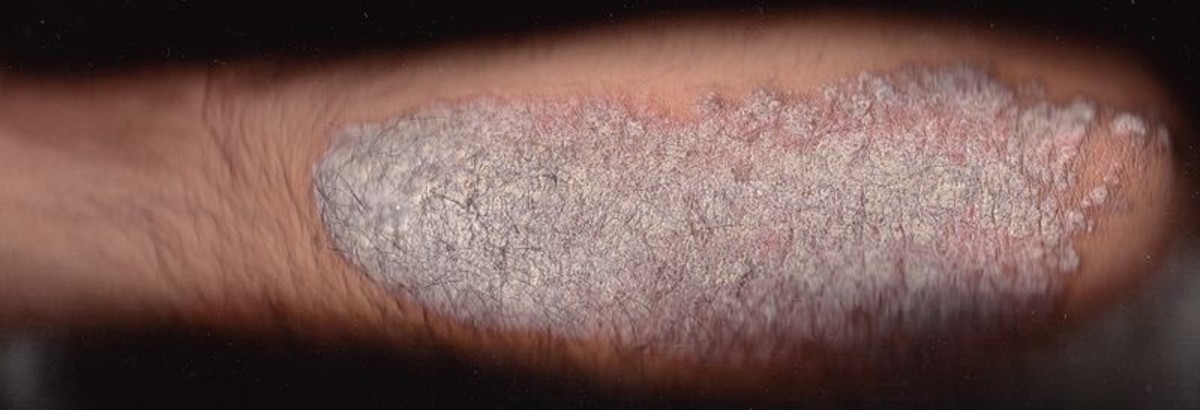
Psoriasis is an autoimmune skin disorder indicated by the rapid increase in skin cell creation. This leaves what is referred to as “plaque” where patches of raised skin appear. The patches appear to be red skin with silvery white dead dry skin on top. These lesions tend to show up on the the scalp, elbows, lower back and knees. In the U.S., there are 4.5 million adults with psoriasis with the people of European ancestry being the ones most likely to be affected.
Autoimmune skin conditions can be treated with antibiotics, immune suppressants, anti-inflammitories and ointments. It is essential to get an accurate diagnosis with any skin disorder so be certain you tell your health practitioner everything about your health since your health history and other disorders that you may have will help with a correct diagnosis. In combination with taking the remedy a general practitioner prescribes for you, you will want to take extra good care of your skin. This calls for using mild soaps, hypoallergenic lotions and limiting UV ray exposure.
You can understand even more articles concerning autoimmune skin conditions and further skincare subjects.